Researchers have developed a technique for coating polymer implants with a bioactive film that significantly increases bonding between the implant and surrounding bone in an animal model. The advance could significantly improve the success rate of such implants, which are often used in spinal surgeries. The work was done by researchers at North Carolina State University, the University of Cambridge and the University of Texas at San Antonio.
The polymer in question is called polyether ether ketone, or PEEK, which has mechanical properties similar to bone, making it attractive for use in spinal implants. However, PEEK doesn’t bond well with bone. To that end, researchers had previously developed a technique for coating PEEK with a substance called hydroxyapatite (HA), which is a calcium phosphate that bonds well with bone. Proof-of-concept studies were promising, but researchers were then only able to apply the HA coating to flat surfaces and had not tested HA-coated implants in an animal model.
“We can now use our technique to coat the entire surface of an implant, and testing HA-coated implants in an animal model has given us very promising results,” says Afsaneh Rabiei, a professor of mechanical and aerospace engineering at NC State and corresponding author of a paper on the work.
The first step of the HA-coating technique – which was developed in Rabiei’s lab – coats a PEEK implant with a thin film of yttria-stabilized zirconia (YSZ). The second step applies a coating of HA. The researchers then heat the HA layer using microwaves. The YSZ layer acts as a heat shield, preventing the PEEK from melting. Meanwhile, the heat gives the HA a crystalline structure that makes it more stable in the body, meaning that the calcium phosphate will dissolve more slowly – promoting bonding with surrounding bone.
In their new study, researchers tested three types of PEEK implants in a rabbit model: PEEK implants with no coating; PEEK implants with an HA coating treated only with microwaves; and PEEK implants with an HA coating treated with both microwaves and brief exposure to an autoclave in order to enhance the HA’s crystalline structure.
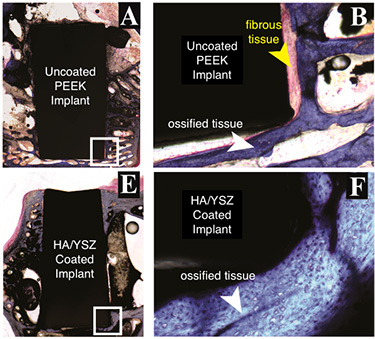
The researchers used microscopic evaluations of tissue cells and three-dimensional X-ray imaging to assess the performance of all three types of implants. Eighteen weeks after surgery, the researchers found that both types of HA-coated implants had more than double the bone formation of PEEK alone, with comparable bone density. The HA-treated implants also had higher bone-to-implant contact ratios than PEEK alone.
“These results indicated an improved implant fixation in the body, decreasing the chances of loosening of the implant after surgery and the need for revision surgery to remove and replace the implant,” Rabiei says. “This improvement is due to increased regenerated bone volume around coated implants compared to uncoated PEEK.”
The researchers also did biomechanical testing on the implants, assessing their “toughness,” or how well the implant bonded to the surrounding bone.
To test this, the researchers conducted what is called biomechanical push-out testing, in which force is applied to an implant until it is dislodged. These results are measured in terms of work as Newton millimeters (N-mm).
At 18 weeks, it took approximately 299.1 N-mm of work to dislodge implants coated with microwave-treated HA and about 312.5 N-mm to dislodge implants coated with microwave and autoclave-treated HA. This compares to about 183.9 N-mm of work needed to dislodge unmodified PEEK implants.
“It is notable that these results were achieved on completely smooth surfaces of PEEK, while our subsequent studies have indicated that by slightly increasing the surface roughness of PEEK prior to coating, we can accomplish even higher adhesion strength of two-layer HA/YSZ coatings that would require even higher work to dislodge,” Rabiei says.
“Whether looking at bone growth or toughness, HA-coated samples outperformed uncoated PEEK implants,” Rabiei says. “This treatment will probably increase the cost of an implant marginally, but should help minimize the need for follow-up surgeries – which means HA-treated implants will more than pay for themselves over time.”
“And the extent of the cost increase remains unclear,” Rabiei adds. “We are not aware of any health risks associated with HA or YSZ – both of which are used in devices already approved by the FDA for long-term implantation. As a result, we may not need additional clinical trials before HA-coated implants can be used in clinical practice. We’re investigating that now, and are looking for industry partners to help us commercialize the technique.”
The paper, “Hydroxyapatite coating on PEEK implants: biomechanical and histological study in a rabbit model,” is published online in the journal Materials Science and Engineering C. Lead author of the paper is John Durham, a postdoctoral researcher at NC State. Co-authors are Matthew Allen of Cambridge; and Sergio Montelongo, Joo Ong and Teja Guda of UT-San Antonio. The work was supported by the National Institute of Dental and Craniofacial Research of the National Institutes of Health under award number R21DE022925.
-shipman-
Note to Editors: The study abstract follows.
“Hydroxyapatite coating on PEEK implants: biomechanical and histological study in a rabbit model”
Authors: John W. Durham III and Afsaneh Rabiei, North Carolina State University; Sergio A. Montelongo, Joo L. Ong, and Teja Guda, University of Texas at San Antonio; and Matthew J. Allen, University of Cambridge
Published: June 15, Materials Science and Engineering C
DOI: 10.1016/j.msec.2016.06.049
Abstract: A bioactive two-layer coating consisting of hydroxyapatite (HA) and yttria-stabilized zirconia (YSZ) was investigated on cylindrical polyether ether ketone (PEEK) implants using ion beam assisted deposition (IBAD). Post-deposition heat treatments via variable frequency microwave annealing with and without subsequent autoclaving were used to crystallize the as-deposited amorphous HA layer. Microstructural analysis, performed by TEM and EDS, showed that these methods were capable of crystallizing HA coating on PEEK. The in vivo response to cylindrical PEEK samples with and without coating was studied by implanting uncoated PEEK and coated PEEK implants in the lateral femoral condyle of 18 rabbits. Animals were studied in two groups 9 for observation at 6 or 18 weeks post surgery. MicroCT analysis, histology, and mechanical pull-out tests were performed to determine the effect of the coating on osseointegration. The heat-treated HA/YSZ coatings showed improved implant fixation as well as higher bone regeneration and bone-implant contact area compared to uncoated PEEK. The study offers a novel method to coat PEEK implants with improved osseointegration.